In healthcare settings, one of the most underestimated yet life-altering risks is a Needlestick Injury (NSI) — also known as a sharps injury. While these incidents may appear minor on the surface, they carry the potential for serious, even fatal, consequences through exposure to Blood-Borne Viruses (BBV).
According to the World Health Organization (WHO), an estimated 2 million healthcare workers experience needlestick injuries every year worldwide, leading to thousands of new infections. In Malaysia alone, healthcare workers remain significantly at risk due to gaps in proper sharp waste management protocols.
Critical Fact: 80% of healthcare workers in Malaysia are exposed to various types of viruses and infections through Needlestick Injuries (NSIs) at some point in their career.
What Is a Needlestick Injury?
A needlestick injury occurs when a needle or other sharp object — such as a lancet, scalpel, or broken glass — accidentally punctures the skin. These incidents most commonly affect:
- Nurses and doctors during injections or blood draws
- Laboratory technicians handling specimen samples
- Surgical staff working with scalpels and suture needles
- Waste disposal workers handling improperly discarded sharps
- Allied health professionals during routine patient care
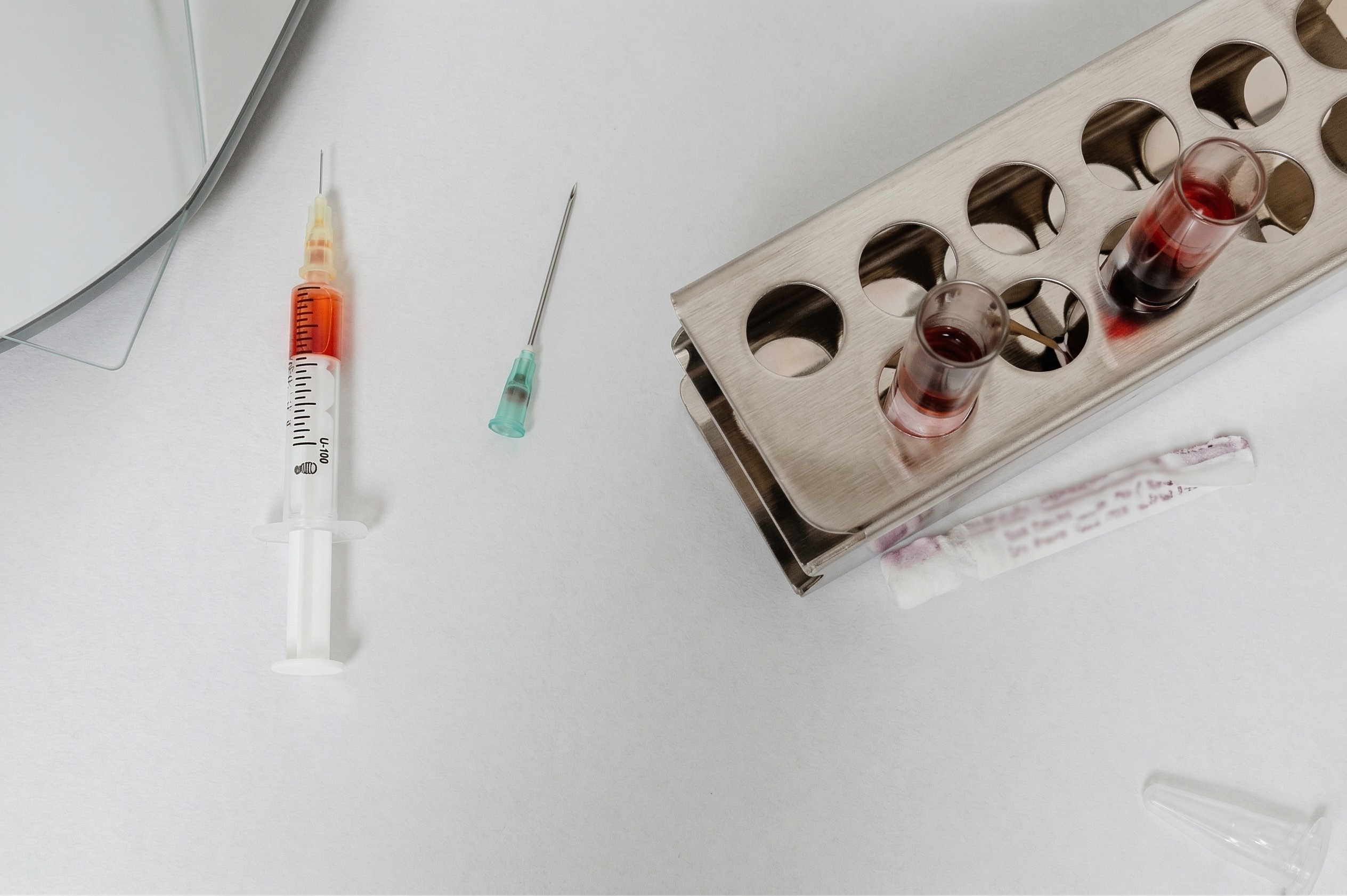
Fig. 1 — Needlestick injuries remain one of the most common occupational hazards in healthcare environments.
Blood-Borne Viruses: The Hidden Danger
The primary concern following a sharps injury is the transmission of Blood-Borne Viruses (BBV). These pathogens are present in infected blood and body fluids, and even a microscopic amount can establish infection. The three most significant BBVs are:
1. Hepatitis B Virus (HBV)
Hepatitis B is the most transmissible of the three BBVs. An unvaccinated healthcare worker exposed to HBV-positive blood faces a 6% to 30% risk of infection depending on the HBeAg status of the source patient. HBV can survive on dry surfaces for up to 7 days, making contaminated equipment particularly dangerous.
The good news: an effective Hepatitis B vaccine exists. All healthcare workers should be fully vaccinated with verified immunity before patient contact.
2. Hepatitis C Virus (HCV)
Unlike HBV, there is currently no vaccine for Hepatitis C. The average risk of HCV transmission after a needlestick from an HCV-positive source is approximately 1.8%. Left untreated, chronic HCV infection can progress to cirrhosis and liver cancer over decades. Early detection following exposure is critical for prompt antiviral treatment.
3. Human Immunodeficiency Virus (HIV)
While HIV has the lowest transmission rate per exposure (0.3%), the consequences of infection are profound. Modern antiretroviral therapy (ART) can suppress the virus to undetectable levels, but there is no cure. Post-Exposure Prophylaxis (PEP) must be initiated within 72 hours of suspected exposure for maximum effectiveness.
| Blood-Borne Virus | Transmission Risk (per NSI) | Vaccine Available | PEP Available |
|---|---|---|---|
| Hepatitis B (HBV) | 6% – 30% | Yes ✓ | Yes (HBIg + vaccine) |
| Hepatitis C (HCV) | ~1.8% | No ✗ | No (monitoring + treatment) |
| HIV | ~0.3% | No ✗ | Yes (ART within 72h) |
Prevention: The First Line of Defence
The most effective strategy against needlestick injuries is prevention at the source. Healthcare institutions must implement a comprehensive sharps safety programme that includes:
- Safe sharps containers — ASTM-certified, puncture-resistant, leak-proof containers placed at point-of-use
- Never recap needles — one-handed technique or a mechanical recapping device only
- Proper disposal training — all staff trained on correct disposal immediately after use
- Engineering controls — use of safety-engineered devices with retractable or shielded needles
- Hepatitis B vaccination — mandatory for all clinical staff with documented immunity verification
- Incident reporting — immediate reporting protocols and post-exposure management plans
Why Certified Sharp Containers Matter
Not all sharp containers are equal. A container that fails — due to puncture, leakage, or inadequate closure — can turn a controlled waste management process into a serious exposure event. ASTM D4169 certification ensures that containers have been tested under real-world conditions including:
- Drop test — simulating accidental falls during transport
- Penetration resistance test — ensuring needles cannot puncture through walls
- Leak resistance test — guaranteeing no liquid can escape
- Closure security test — permanent closure once sealed

Fig. 2 — YM Medic Sharp Container, ASTM D4169 certified for maximum sharps containment safety.
YM Medic Sdn Bhd's sharp containers are designed with all six critical safety features: translucent rigid walls, tight-fitting lids, leak-resistant construction, clear fill lines, permanent closure mechanisms, and one-handed user-friendly design — ensuring healthcare workers can dispose of sharps safely every time.
Immediate Steps After a Sharps Injury
If a needlestick injury occurs, act immediately:
- Wash the wound thoroughly with soap and running water for at least 2 minutes
- Do not squeeze or suck the wound — allow natural bleeding
- Apply antiseptic and cover with a waterproof dressing
- Report the incident to your supervisor and occupational health department immediately
- Seek medical assessment within hours — especially for HIV PEP (must begin within 72h)
- Identify source patient's BBV status if possible and consent obtained
- Follow up with serology testing at recommended intervals
Remember: Every sharps injury must be formally reported. Under-reporting prevents institutions from identifying risk patterns and implementing corrective safety measures.
Conclusion
The risk from a sharps injury extends far beyond a moment of pain — it represents a potential life-changing exposure to serious infectious diseases. Healthcare institutions have a duty of care to protect their staff through proper equipment, training, and protocols. The use of certified sharp containers, combined with safe handling practices and a strong reporting culture, can dramatically reduce the incidence of needlestick injuries and the human cost that comes with them.
At YM Medic Sdn Bhd, we are committed to manufacturing sharps containers that meet the highest international standards, because we believe no healthcare worker should face preventable infection risk.

.png)

Leave a Comment
Share your thoughts or questions